The Strongest Predictor of Heart Attack Isn't a Cholesterol Test
I tested 12 biomarkers head-to-head. The winner surprised me.
Half of all heart attacks happen to people with LDL below 100 mg/dL — the level that federal cholesterol guidelines classified as “optimal.”[1]
That number should stop the cardiovascular prevention industry in its tracks. It doesn’t. The field remains fixated on lipids (the fats in your blood) while largely ignoring the other half: chronic inflammation.
It follows directly from how heart disease develops — a two-step process most people never hear explained clearly.
Step one: cholesterol gets trapped. LDL (low-density lipoprotein) particles pass through your artery walls every day. Most pass back out. But at branches and curves — areas of turbulent flow — some get stuck.
Step two: your immune system makes it worse. Your body treats trapped particles as a threat and sends immune cells to clean them up. Those cells gorge on cholesterol, die, and pile up — forming plaque inside the artery wall. That’s inflammation growing the deposit. But the same immune response also weakens the plaque’s shell from inside. Over years, this weakening continues until the shell ruptures, triggering a clot. That clot is a heart attack or stroke.
Plaque Doesn’t Kill You — Rupture Does
A large, stable plaque can sit in an artery wall for decades without causing a heart attack. It’s the inflamed, thin-capped plaque that blows. Inflammation does two things: it builds the plaque and it destabilizes it. More inflammation means faster growth and higher rupture risk. Both steps — trapping and inflammation — are necessary. But the entire clinical apparatus points at only the first. This is why CRP (C-reactive protein, a blood marker of inflammation) predicts heart attacks even when cholesterol looks fine — and why walking, which crushes inflammation, produces cardiovascular benefits that cholesterol drugs can’t match.
I started researching this post to answer a simple question: which cholesterol measure matters most? The field has been refining this since Framingham began tracking cholesterol in 1948:
Total cholesterol: the original measure — just one number, tracked since the 1950s
The lipid panel: the standard blood test since the 1980s, breaking cholesterol into three parts:
LDL: the fraction that builds plaque
HDL (high-density lipoprotein): thought to clear it
Triglycerides: blood fats linked to metabolic health
ApoB: a protein on LDL particles, considered a more precise count of the particles that build plaque. Gaining traction since the 2000s
Lp(a): a genetically determined lipoprotein linked to clotting risk. Discovered in 1963, but only entered major clinical guidelines around 2019
Each new marker spawns a new drug target, a new guideline, a new debate. I expected to find that one of them — probably ApoB — was the clear winner for predicting cardiovascular risk.
Instead, I found that the single most actionable marker for cardiovascular risk wasn’t a cholesterol measure at all. It was CRP — or more precisely, its high-sensitivity version, hs-CRP. CRP was discovered in the 1930s, but the standard assay could only detect levels above 3 mg/L — enough for infections, useless for cardiovascular risk. The high-sensitivity version became clinically available in the late 1990s. (Same protein — “high-sensitivity” just means the lab uses a more precise assay. I’ll just call it CRP from here.)
No joke. This is Framingham, Massachusetts of the Framingham study! Photo by Omri D. Cohen on Unsplash
The 20-Year Accident
HDL entered the standard lipid panel in the early 1980s. The hs-CRP assay didn’t arrive until the late 1990s. For roughly twenty years, HDL was on every blood panel in the country while low-grade inflammation was unmeasurable. During that window, a doctor seeing “high HDL” was often seeing low inflammation — but attributing it to cholesterol transport. We now know inflammation remodels HDL particles, replacing their functional proteins with inflammatory ones.[2] The number on the blood test was tracking inflammation, not cholesterol.
When Paul Ridker — a cardiologist at Brigham and Women’s Hospital who has spent three decades building the case for inflammation in cardiovascular disease — finally measured both simultaneously in 28,263 healthy women, the overlap became obvious.[3] Of twelve biomarkers tested one at a time, CRP was the strongest predictor of cardiovascular events — women in the top quarter for CRP had 4.4x the risk of those in the bottom quarter. When all twelve were tested together, adjusting for age, smoking, obesity, hypertension, diabetes, and family history, only two independently predicted risk: CRP (1.5x) and the total cholesterol/HDL ratio (1.4x). Every other biomarker, including LDL, dropped out. The only lipid measure that survived had HDL in the denominator — inadvertently capturing the same inflammatory signal CRP measured directly.
So was high HDL actually protecting people, or was it just a sign of low inflammation? The drug trials answered that. Multiple attempts to raise HDL pharmacologically failed[4]:
Torcetrapib: +72% HDL, increased mortality
Dalcetrapib: +30% HDL, no benefit
Evacetrapib: +130% HDL, no benefit
HDL wasn’t protecting anyone. It was reflecting low inflammation. CRP measured the same thing directly.
The Evidence
Three studies separated CRP’s effect from LDL’s — in clinical trials, in population data, and with a drug that only targets inflammation.
JUPITER (18,000 people, normal LDL, elevated CRP): Rosuvastatin lowered both LDL and CRP simultaneously, but the reductions were weakly correlated in individual patients — making it possible to separate the effects.[5] Patients who hit the LDL target saw a 55% reduction in cardiovascular events. Those who hit the CRP target saw 62%. Same drug, same trial — CRP reduction mattered more.[6] The 10% who drove CRP below 1 mg/L saw a 79% reduction in cardiovascular events.[7]
CANTOS (10,000 post-heart-attack patients): Canakinumab reduced CRP by 37% without touching LDL at all. Cardiovascular events dropped 15–27%.[8] You can reduce cardiovascular events by targeting inflammation alone, without changing cholesterol by a single point.
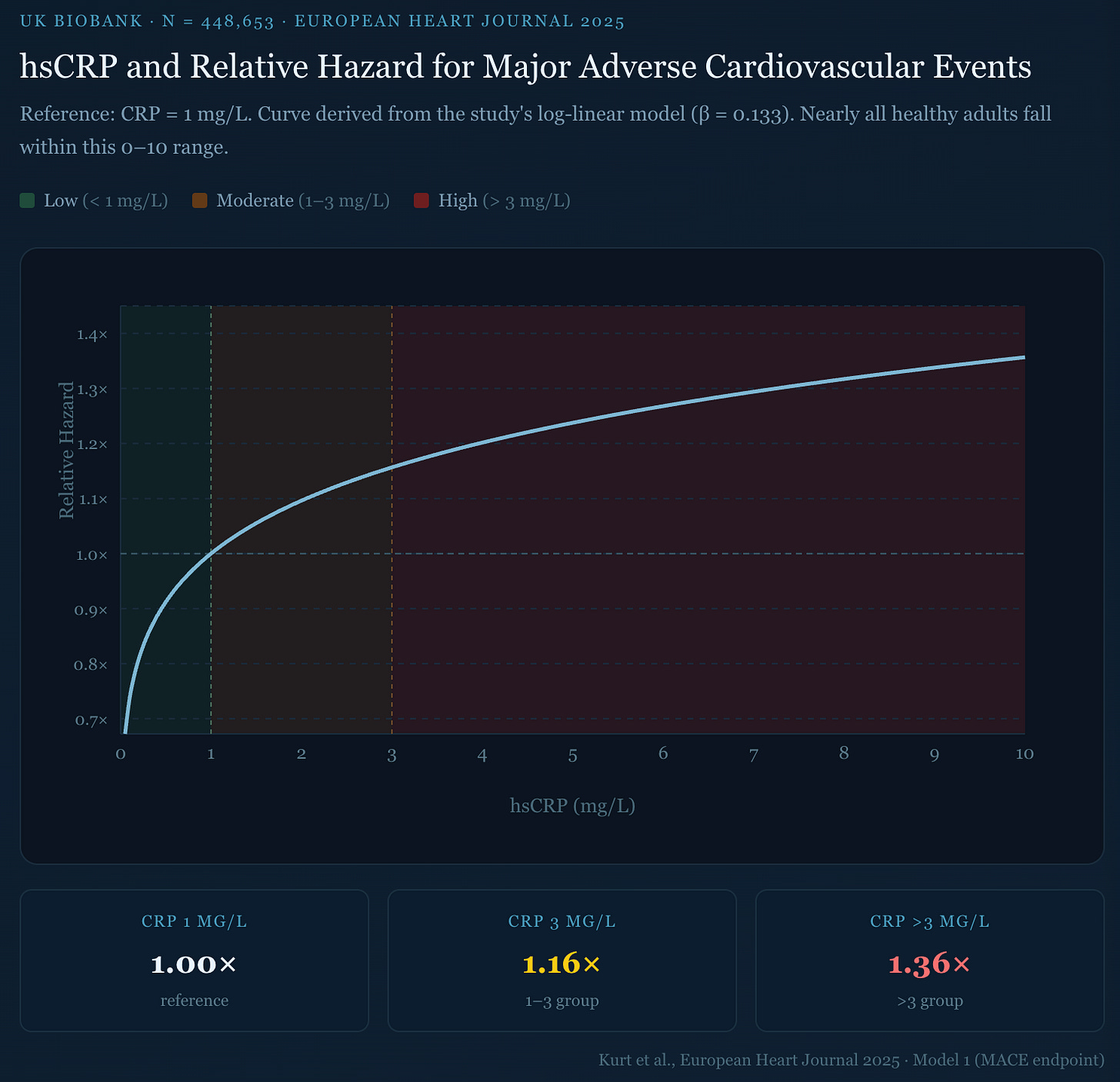
UK Biobank (450,000 people, general population): CRP above 3 mg/L meant 61% higher cardiovascular death — after adjusting for every standard risk factor including LDL.[9] Even among people with zero conventional risk factors — no hypertension, no diabetes, no abnormal cholesterol, no smoking — CRP still separated who had events from who didn’t.
So Why Hasn’t This Changed Anything?
The infrastructure that decides which blood test your doctor orders traces back to Framingham. By the 1960s it had identified high cholesterol as a major cardiovascular risk factor. By the 1970s it had established LDL as “bad” and HDL as “good.” The risk calculators, treatment guidelines, and drug targets that followed were all built on this framework — and when statins arrived in 1987, the field had its perfect tool: a drug that moved the number Framingham said mattered most. That original model is now nearly 80 years old. It has been refined, but never fundamentally questioned. The major risk calculators still in clinical use descend from it.
Count the tools aimed at the lipid side: LDL targets. ApoB goals. Statins — cholesterol-lowering drugs prescribed to over 200 million people worldwide.[10] PCSK9 inhibitors (a newer class of injectable cholesterol drugs) at $5,800+/year. Ezetimibe. Bempedoic acid. Inclisiran. And now the race to develop Lp(a)-lowering drugs.
Now count the tools aimed at the inflammatory side: almost nothing. Statins lower CRP — rosuvastatin drops it by about 48% — but they’re prescribed for LDL, marketed for LDL, and dosed by LDL targets. The CRP reduction is treated as a side effect, not the point — which may explain why statins outperform other lipid-lowering drugs that don’t touch inflammation. The one drug that specifically targets cardiovascular inflammation (canakinumab) was denied FDA approval because it increased fatal infections. No clinical guidelines set CRP targets. The AHA and CDC issued a joint statement on CRP screening in 2003, but gave it a Class IIb recommendation — the weakest possible endorsement, meaning “may be reasonable.”[11] For comparison, LDL testing carries a Class I — “should be performed.” That gap in endorsement means many doctors simply don’t order the test.
Why CRP Moves Faster
The intervention side mirrors the testing side. Just as measurement fixated on LDL when CRP was the stronger predictor, treatment fixated on diet and drugs that move LDL. Diet shifts LDL by roughly 5–15%.[12] Real but modest. Moving LDL further requires medication, and even intensive statin therapy only shrinks plaque by ~1% per year. That’s a slow process.
CRP responds faster. Exercise interventions produce measurable CRP drops within 4–8 weeks.[13] CRP’s half-life is roughly 19 hours — once you remove the inflammatory trigger, it clears quickly. People who sustain higher walking volume don’t just temporarily suppress CRP; they reset to a lower baseline. The body shifts from a chronic inflammatory state to a non-inflammatory one in months, not years.
You don’t need to reverse decades of atherosclerosis to reduce your near-term risk of a cardiac event. You need to stop destabilizing the plaque you already have. Walking does that on a timeline measured in weeks, not years.
Walking Crushes Inflammation
All exercise lowers CRP — aerobic, resistance, and combined training all produce comparable reductions.[14][15] The reductions are large enough to shift people between the clinical risk categories the UK Biobank study just validated.
Walking’s advantage isn’t that it’s better per minute — it’s that you can do so much more of it. Yates et al. found that people walking ~10,000 daily steps had CRP roughly 1.8 mg/L lower than those at ~2,000 — enough to move someone from high-risk (above 3 mg/L) to low.[16] Volume drove the effect, not intensity.
But the real story isn’t “exercise lowers CRP.” It’s that walking produces the largest cardiovascular mortality reduction ever documented — and CRP is the biomarker that tracks it.
The Banach meta-analysis — 17 studies, nearly 227,000 participants — tracked daily steps against cardiovascular mortality.[17] People walking ~10,000 steps/day had a 77% reduction in CV death versus those at ~2,300. Every additional 500 steps cut CV mortality by 7%.
A 77% reduction in cardiovascular death. For comparison, running — a more intense activity — is associated with a ~30% CVD mortality reduction in a meta-analysis of 232,000 people.[18] Strength training: ~19%.[19] Both are valuable — but neither comes close to the walking number, because neither can match the volume. You can walk two hours a day, every day, for decades. You can’t run or lift that way.
Step intensity didn’t matter after adjusting for volume.[20] It’s the volume, not the speed.
This aligns with walking’s S-tier ranking in the longevity framework. Walking hits all three systems: vascular (blood pressure, artery function), immune (CRP), and metabolic (insulin sensitivity, blood sugar regulation).
What This Looks Like in Practice
My CRP is 0.05 mg/L — at the detection limit. I don’t take statins. I don’t take anti-inflammatory supplements. I walk 20,000 steps per day.
To put that in context: rosuvastatin in JUPITER dropped CRP by about 2 mg/L in absolute terms (from 4.2 to 2.2). The Yates dose-response data predicts a similar ~1.8 mg/L drop from going from 2,000 to 10,000 daily steps. In raw CRP reduction, walking roughly matches a statin — plus everything else it does for blood pressure, insulin sensitivity, and muscle preservation.
My LDL is 98 mg/dL and ApoB is 90 mg/dL — normal but not dramatically low. A lipid-focused physician might want to prescribe a statin. My inflammation markers suggest I’m already addressing the higher-risk side of the equation.
The Simple Math
Test your CRP. Below 1.0 mg/L, you’re doing something right. Above 2.0, you have a modifiable risk factor that walking addresses directly — and that most risk calculators are ignoring.
If LDL is the fuel of atherosclerosis, inflammation is the spark. Medicine spent 80 years lowering the fuel. Walking removes the spark.
Walk more. Measure CRP. Lower both halves of the risk equation.
References
Rosuvastatin to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein
Antiinflammatory Therapy with Canakinumab for Atherosclerotic Disease
C-reactive protein and cardiovascular risk in the general population
Effect of exercise training on C reactive protein: a systematic review and meta-analysis
Role of exercise in lowering CRP: a meta-analysis of meta-analyses
The anti-inflammatory effects of exercise training in patients with cardiovascular disease
Dose-response association between step count and cardiovascular disease risk markers
The association between daily step count and all-cause and cardiovascular mortality
Is running associated with a lower risk of all-cause, cardiovascular and cancer mortality?
Resistance Training and Mortality Risk: A Systematic Review and Meta-Analysis
Association of Daily Step Count and Step Intensity With Mortality Among US Adults